Congestive heart failure diagnosis and treatment / and A case of Heart Failure
IMPORTANT NOTE: THE SITE IS UNDER DEVELOPMENT AND CONTENTS ARE CONTINUOUSLY ADDED.
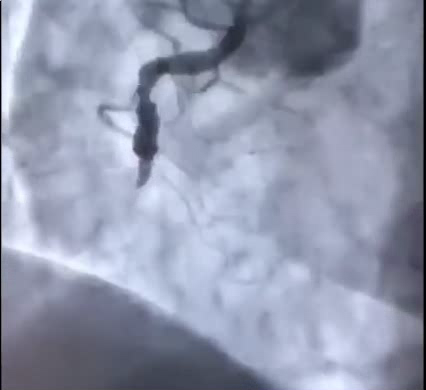
One of my medical videos. A case of ischemic cardiomyopathy The patient presented with effort dyspnea, in the context of coronary artery disease and a previous myocardial infarction. The ECG, the echocardiogram, the myocardial perfusion scan (SPECT) and the coronary angiography of the patient are presented and the appropriate treatment is discussed.
NOTES
Definition of heart failure and general considerations
Definition: Heart failure (HF) is a progressive pathologic condition. It is defined as a clinical syndrome that results from any structural or functional abnormality of the heart resulting in a reduced cardiac output and/ or elevated intracardiac pressures at rest or during stress (physical activity) and is characterized by typical symptoms (e.g. breathlessness, ankle swelling and fatigue) and/or signs (e.g. elevated jugular venous pressure, pulmonary crackles and peripheral oedema). HF can also be defined as an abnormality of cardiac structure or function that impairs the ability of the left ventricle, or the right ventricle, or both ventricles, to eject blood, or to fill with blood, leading to failure of the heart to deliver blood and oxygen at a rate commensurate with the requirements of the metabolizing tissues, despite normal filling pressures, or the situation in which the heart is able to deliver to the tissues, blood and oxygen at a sufficient rate only at the expense of increased filling pressures. HF may involve the left heart, the right heart, or be biventricular.HF is characterized by dyspnea and/or fatigue on exertion (and occasionally at rest) and evidence of fluid retention, which can manifest as peripheral edema or pulmonary congestion. Clinically HF can be defined, as a syndrome in which patients have typical symptoms (e.g. breathlessness, ankle swelling, and fatigue) and signs (e.g. elevated jugular venous pressure, pulmonary crackles, and displaced apex beat), resulting from an abnormality of cardiac structure or function.
The prevalence of HF is increasing. The prognosis is severe for symptomatic HF (50 % or more of patients hospitalized for heart failure die within the next 5 years.) HF is a significant cause of morbidity and mortality. Death in HF can occur as sudden cardiac death (due to the sudden occurrence of a ventricular tachyarrhythmia: ventricular tachycardia or ventricular fibrillation), or as a result of end stage HF with worsening heart failure symptoms and fluid overload.
Many of the signs of HF result from sodium and water retention and resolve quickly with diuretic therapy.
Very important for the diagnosis of HF is demonstration of an underlying cardiac cause This is usually myocardial disease causing systolic ventricular dysfunction (for example ischemic cardiomyopathy in the context of a previous myocardial infarction, dilated cardiomyopathy). However, abnormalities of ventricular diastolic function or of the valves (for example severe aortic or mitral valve disease, severe stenosis of the pulmonary valve,etc), pericardium (for example constrictive pericarditis), endocardium, heart rhythm (heart failure due to a tachyarrhythmia), and conduction (heart failure caused by serious bradycardia,advanced atrioventricular block) can also cause HF. Occasionally, more than one abnormality can be present.
Systolic HF, or heart failure with reduced ejection fraction
Systolic HF, or HF with reduced ejection fraction, is due to an impaired left ventricular systolic function: It is a failure of the left ventricle to eject blood in order to maintain a cardiac output adequate to meet the total metabolic needs of the body, under normal ventricular filling pressures. The cardiac output can be reduced (manifestations of inadequate cardiac output are fatigue on exertion, or even hypotension and shock) or more commonly cardiac output may be normal, but under the expense of abnormally elevated ventricular filling pressures, causing the manifestations of congestion (effort dyspnea, nocturnal dyspnea and orthopnea, acute pulmonary edema, pleural effusion, peripheral edema, hepatomegaly, jugular venous distention, etc.). Systolic HF is caused by damage to the cardiac muscle (myocardium) from infarction, inflamation (myocarditis), toxicity (alcohol, chemotherapeutic drugs used for the treatment of malignancies), chronic pressure overload (chronic hypertension, severe aortic valve stenosis), chronic volume overload ( severe aortic or mitral regurgitation, large cardiac shunts due to congenital heart disease), etc.According to the recent guidelines (ESC 2016) HF with reduced EF is defined by the presence of symptoms and/or signs of HF in patients with left ventricular EF <40 % .
Diastolic HF, or heart failure with preserved ejection fraction (EF)
Diastolic HF, or HF with preserved ejection fraction (EF): However, there is also a large group of patients with signs and symptoms of heart failure, but apparently preserved left ventricular systolic function, with left ventricular ejection fraction ≥ 50%. These patients have diastolic HF or HF with preserved ejection fraction (EF). The latter term is better, because often patients with this type of HF, do not have a completely normal systolic function, when they are examined with more sensitive tests, such as tissue Doppler echocardiography or myocardial strain imaging. These sensitive tests show that these patients usually also have subtle abnormalities of systolic function. The important fact is, that in these patients the predominant disorder, causing the manifestations of HF, is a disorder of the ventricular diastolic function. In simple words, there is an abnormality in the ability of the left ventricle to fill in diastole, causing elevated filling pressures and manifestations of pulmonary congestion (effort dyspnea, nocturnal dyspnea, orthopnea, even acute pulmonary edema). The severe impairment of diastolic function may be transient (e.g. acute ischemia) or persistent ( e.g. left ventricular hypertrophy due to hypertension, or hypertrophic cardiomyopathy /restrictive or infiltrative cardiomyopathy/ diabetic cardiomyopathy).Recent guidelines (ESC 2016) define HF with preserved EF by the following criteria:
(a) Patients with symptoms and /or signs of HF,
(b) left ventricular EF ≥ 50%,
(c) elevated natriuretic peptide (BNP> 35 pg/ml or NTProBNP> 125 pg/ml) and
(d) at least one of the following:
Evidence of a relevant structural heart disease (e.g. left ventricular hypertrophy, left atrial enlargement), or
Evidence of diastolic dysfunction (usually obtained with echocardiography).
Heart failure with mid-range EF
Recent guidelines also define a form of HF between HF with reduced and HF with preserved EF. This is:HF with mid-range EF and it is defined by the following criteria:
Patients with symptoms and /or signs of HF,
left ventricular EF between 40 and 50 % (41-49%) plus the criteria (c) and (d) mentioned above for HF with preserved EF.
The symptoms of these patients most probably are caused primarily by mild systolic dysfunction, or by a combination of diastolic and systolic dysfunction.
Stage A: People without significant structural heart disease, being at risk for future development of heart failure, based on the presence of risk factors such as hypertension, atherosclerotic disease, diabetes mellitus, prior exposure to cardiotoxic agents (such as doxorubicin), or a family history of a cardiomyopathy. These predisposing factors do not constitute the syndrome of heart failure, so the importance of this stage is to emphasize the need for early identification of individuals with risk factors for a better follow up and for treatment of any modifiable risk factors.
left ventricular EF between 40 and 50 % (41-49%) plus the criteria (c) and (d) mentioned above for HF with preserved EF.
The symptoms of these patients most probably are caused primarily by mild systolic dysfunction, or by a combination of diastolic and systolic dysfunction.
Stages of heart failure
This staging classification has been adopted by the guidelines with the purpose to emphasize the progressive nature and the evolution of heart disease leading to the development of HF.Stage A: People without significant structural heart disease, being at risk for future development of heart failure, based on the presence of risk factors such as hypertension, atherosclerotic disease, diabetes mellitus, prior exposure to cardiotoxic agents (such as doxorubicin), or a family history of a cardiomyopathy. These predisposing factors do not constitute the syndrome of heart failure, so the importance of this stage is to emphasize the need for early identification of individuals with risk factors for a better follow up and for treatment of any modifiable risk factors.
Stage B includes patients with structural heart disease, but without signs or symptoms of heart failure (HF), such as patients with
previous myocardial infarction, low ejection fraction (EF), left ventricular hypertrophy, or asymptomatic valvular disease.Patients with asymptomatic left ventricular systolic dysfunction (of ischemic or nonischemic etiology) should receive an ACE inhibitor to reduce of developing symptomatic heart failure and death. If there is an intolerance to an ACE- inh because of cough or angioedema, an angiotensin receptor blocker- ARB( especially valsartan) is an effective treatment alternative. In patients with left ventricular dysfunction in the context of a myocardial infarction, the combination of an ACE inhibitor and ARB is not better than either alone, so in this setting, combination therapy is not recommended.
Beta -blockers in patients with a recent myocardial infarction and reduced left ventricular EF (≤40%) also improve survival and reduce subsequent nonfatal myocardial infarctions, when added to an ACE inhibitor.
Stage C: Patients with structural heart disease with prior or current symptoms of HF (e.g. shortness of breath, fatigue, reduced exercise tolerance, edema)
Usual treatment includes diuretics for fluid retention (symptoms and signs of congestion) and for patients with stage C heart failure with reduced left ventricular EF drug cate proven by randomized trials to reduce mortality (and also reduce hospitalizations): ACE inhibitors (or ARBs) beta- blockers, mineralocorticoid antagonists. (See below, the chapter on treatment and the links to the guidelines).
Stage D
Refractory HF requiring specialized interventions. Patients with end stage (stage D) heart failure have the following characteristics: severe symptoms at rest or with minimal activity despite optimal medical treatment, recurrent decompensation with hospitalizations, severe cardiac dysfunction and often a need for treatment with inotropes. Besides optimal medical treatment, with the drugs used for stage C, these patients often require treatment in specialized centers and for some of them, advanced forms of treatment are required (such as chronic-permanent mechanical circulatory assist devices, heart transplantation, treatment with intravenous inotropic medications).
previous myocardial infarction, low ejection fraction (EF), left ventricular hypertrophy, or asymptomatic valvular disease.Patients with asymptomatic left ventricular systolic dysfunction (of ischemic or nonischemic etiology) should receive an ACE inhibitor to reduce of developing symptomatic heart failure and death. If there is an intolerance to an ACE- inh because of cough or angioedema, an angiotensin receptor blocker- ARB( especially valsartan) is an effective treatment alternative. In patients with left ventricular dysfunction in the context of a myocardial infarction, the combination of an ACE inhibitor and ARB is not better than either alone, so in this setting, combination therapy is not recommended.
Beta -blockers in patients with a recent myocardial infarction and reduced left ventricular EF (≤40%) also improve survival and reduce subsequent nonfatal myocardial infarctions, when added to an ACE inhibitor.
Stage C: Patients with structural heart disease with prior or current symptoms of HF (e.g. shortness of breath, fatigue, reduced exercise tolerance, edema)
Usual treatment includes diuretics for fluid retention (symptoms and signs of congestion) and for patients with stage C heart failure with reduced left ventricular EF drug cate proven by randomized trials to reduce mortality (and also reduce hospitalizations): ACE inhibitors (or ARBs) beta- blockers, mineralocorticoid antagonists. (See below, the chapter on treatment and the links to the guidelines).
Stage D
Refractory HF requiring specialized interventions. Patients with end stage (stage D) heart failure have the following characteristics: severe symptoms at rest or with minimal activity despite optimal medical treatment, recurrent decompensation with hospitalizations, severe cardiac dysfunction and often a need for treatment with inotropes. Besides optimal medical treatment, with the drugs used for stage C, these patients often require treatment in specialized centers and for some of them, advanced forms of treatment are required (such as chronic-permanent mechanical circulatory assist devices, heart transplantation, treatment with intravenous inotropic medications).
The NYHA classification of heart failure (HF)
The New York Heart Association (NYHA) classification is a scale used for classifying patients with HF according to the severity of symptoms and has prognostic and therapeutic implications:
NYHA I: asymptomatic
NYHA II: symptomatic with moderate exertion
NYHA III: symptomatic with mild exertion and may limit activities of daily living
NYHA IV: symptomatic at rest.
Is it possible to classify patients with heart failure (HF), especially those with acute HF, into hemodynamic categories according to their clinical manifestations, and can this influence the treatment strategy?
Yes...The manifestations (signs and symptoms) of HF can be classified into those caused by low perfusion (i.e., "cool" hemodynamics) and those caused by congestion (increased pulmonary and systemic venous pressure and salt and water retention = "wet hemodynamics").
The manifestations of low perfusion (decreased cardiac output=is decreased volume of blood passing through the circulation per minute) are the following:
Decreased pulse pressure (pulse pressure = systolic pressure –diastolic pressure), cool extremities, altered mental status and decreased urine output. Some or all of these manifestations can be present depending on the severity of the patient's condition.
The manifestaitons of congestion (i.e., wet hemodynamics) can be some or all of the following :
Dyspnea on exertion, paroxysmal nocturnal dyspnea, orthopnea, edema, elevated jugular venous pressure (external jugular veins become distended and the pulsations of the internal jugular vein are visible at an increased height, measured from the sternal angle), ascites (abdomimal distention due to the accumulation of fluid), an audible third heart sound at early diastole, crackles on lung auscultation, hepatojugular reflux.
A practical, simplified, approach is to classify the patient with HF into one of the following hemodynamic profiles:
Warm and dry: the patient is well compensated, with no manifestations of low tissue perfusion or congestion. No change in medical management is needed on the basis of the clinical manifestations.
Warm and wet: The patient is congested but has no manifestations of decreased perfusion. Diuretic treatment should be increased to reduce congestion.
Cool and dry: The patient has manifestations of diminished perfusion, but no manifestations of congestion. A general rule is to add inotropic support to improve perfusion, especially if the manifestations are severe, but also the dosage of vasodilators such as ACE inhibitors can be increased (with caution to avoid hypotension), in order to reduce afterload and hence increase cardiac output.
Cool and wet: The patient has manifestations of diminished perfusion as well as manifestations of congestion. A general rule is to increase diuretic therapy, to treat congestion and add inotropic support (especially if the patient has severe signs of diminished perfusion or significant hypotension).
The above classification is simplified and schematic, but it is often helpful, especially in some cases of acute heart failure. We should emphasize that the cornerstone of the treatment of HF with reduced EF (systolic HF) is formed by those medications proved in major clinical trials to increase survival: angiotensin converting enzyme inhibitors (ACE-inhibitors) or angiotensin receptor blockers (ARBs), beta-blockers and aldosterone antagonists.
The chest x -ray is a simple and widely available imaging study that can provide some important clues, but the most useful study in a patient with suspected or known HF is echocardiography.
The chest X-ray of a male patient, 60 years old, ex-smoker (15 pack-years), with no history of increased alcohol consumption and with no previous history of cardiac or respiratory disease. He presented with effort dyspnea class NYHA-3 in the last 2 months and a general feeling of tiredness. The physical examination revealed no significant findings, other than reduced intensity of heart sounds. Auscultation of the lungs was also normal. Is the shortness of breath most probably due to a cardiac or a respiratory disorder? What further testing is indicated ?

THE ANSWER
Findings include enlargement of the hilar shadows, dilatation of the lung vessels and more prominent vascular markings in the upper lung fields. These are signs suggestive of elevated pulmonary venous pressure due to heart disease. In contrast there are no findings indicative of a pulmonary disease. Increased dimensions of the cardiac shadow are also observed with an increased prominence of the lower portion of its left margin. The latter finding suggests dilatation of the left ventricle (LV). These findings in conjunction with the presenting symptom of effort dyspnea favor the diagnosis of heart failure (HF), the cause and the severity of which can be investigated by means of further tests. An ECG and an echocardiogram are absolutely mandatory. According to the ESC guidelines (2016) the following laboratory tests are recommended for a patient with newly diagnosed HF in order to evaluate the patient’s suitability for particular therapies and to detect treatable causes and comorbidities: Hemoglobin and WBC - urea, creatinine (with estimated GFR), sodium, potassium, - glucose, HbA1c --lipid profile- liver function tests (AST, ALT, bilirubin,GGT) TSH - ferritin. Natriuretic peptides can also be cosidered as a part of the evaluation. Depending on the findings and the pretest probability of coronary artery disease (risk factors), coronary angiography is often indicated in cases of HF, especially with LV systolic dysfunction, to confirm or exclude coronary artery disease, as a common underlying cause.
On echocardiography this patient had a dilated and diffusely hypokinetic LV with an EF 35 % and also a dilated left atrium. The right heart chambers and the valves were without significant abnormalities (appart from moderate functional mitral regurgitation). Coronary angiography did not reveal significant coronary arterial stenoses. He was diagnosed with HFrEF due to dilated cardiomyopathy and treated with an ACE inhibitor (quinapril), a beta blocker (carvedilol), an MRA (eplerenone) and a loop diuretic (furosemide). Symptoms resolved and on re-evaluation after three months of treatment his EF had improved (40 %) and the dilatation of the LV had decreased. Subsequently, the dosage of the diuretic was reduced and the dosage of the ACE inhibitor was increased.
In the posteroanterior chest radiograph the right border of the cardiomediastinal shadow is formed (from its lower to its upper parts), by the right atrium, the ascending aorta, and superior vena cava and further cranially it widens into a funnel shape, where its right border is formed by the brachiocephalic trunk. The upper margin of the left cardiomediastinal silhouette (from its upper to its lower portions) is formed by the aortic arch, the left pulmonary artery and the atrial appendage. The lower part of the left cardiomediastinal silhouette is formed by the left ventricle. The contour of the left hemidiaphragm is visible through the heart shadow almost as far as the shadow of the vertebral column.
A practical clinical classification of patients with heart failure
Is it possible to classify patients with heart failure (HF), especially those with acute HF, into hemodynamic categories according to their clinical manifestations, and can this influence the treatment strategy?
Yes...The manifestations (signs and symptoms) of HF can be classified into those caused by low perfusion (i.e., "cool" hemodynamics) and those caused by congestion (increased pulmonary and systemic venous pressure and salt and water retention = "wet hemodynamics").
The manifestations of low perfusion (decreased cardiac output=is decreased volume of blood passing through the circulation per minute) are the following:
Decreased pulse pressure (pulse pressure = systolic pressure –diastolic pressure), cool extremities, altered mental status and decreased urine output. Some or all of these manifestations can be present depending on the severity of the patient's condition.
The manifestaitons of congestion (i.e., wet hemodynamics) can be some or all of the following :
Dyspnea on exertion, paroxysmal nocturnal dyspnea, orthopnea, edema, elevated jugular venous pressure (external jugular veins become distended and the pulsations of the internal jugular vein are visible at an increased height, measured from the sternal angle), ascites (abdomimal distention due to the accumulation of fluid), an audible third heart sound at early diastole, crackles on lung auscultation, hepatojugular reflux.
A practical, simplified, approach is to classify the patient with HF into one of the following hemodynamic profiles:
Warm and dry: the patient is well compensated, with no manifestations of low tissue perfusion or congestion. No change in medical management is needed on the basis of the clinical manifestations.
Warm and wet: The patient is congested but has no manifestations of decreased perfusion. Diuretic treatment should be increased to reduce congestion.
Cool and dry: The patient has manifestations of diminished perfusion, but no manifestations of congestion. A general rule is to add inotropic support to improve perfusion, especially if the manifestations are severe, but also the dosage of vasodilators such as ACE inhibitors can be increased (with caution to avoid hypotension), in order to reduce afterload and hence increase cardiac output.
Cool and wet: The patient has manifestations of diminished perfusion as well as manifestations of congestion. A general rule is to increase diuretic therapy, to treat congestion and add inotropic support (especially if the patient has severe signs of diminished perfusion or significant hypotension).
The above classification is simplified and schematic, but it is often helpful, especially in some cases of acute heart failure. We should emphasize that the cornerstone of the treatment of HF with reduced EF (systolic HF) is formed by those medications proved in major clinical trials to increase survival: angiotensin converting enzyme inhibitors (ACE-inhibitors) or angiotensin receptor blockers (ARBs), beta-blockers and aldosterone antagonists.
Imaging in heart failure ( Chest radiography / Echocardiography)
The chest x -ray is a simple and widely available imaging study that can provide some important clues, but the most useful study in a patient with suspected or known HF is echocardiography.
The chest X-ray of a male patient, 60 years old, ex-smoker (15 pack-years), with no history of increased alcohol consumption and with no previous history of cardiac or respiratory disease. He presented with effort dyspnea class NYHA-3 in the last 2 months and a general feeling of tiredness. The physical examination revealed no significant findings, other than reduced intensity of heart sounds. Auscultation of the lungs was also normal. Is the shortness of breath most probably due to a cardiac or a respiratory disorder? What further testing is indicated ?

Findings include enlargement of the hilar shadows, dilatation of the lung vessels and more prominent vascular markings in the upper lung fields. These are signs suggestive of elevated pulmonary venous pressure due to heart disease. In contrast there are no findings indicative of a pulmonary disease. Increased dimensions of the cardiac shadow are also observed with an increased prominence of the lower portion of its left margin. The latter finding suggests dilatation of the left ventricle (LV). These findings in conjunction with the presenting symptom of effort dyspnea favor the diagnosis of heart failure (HF), the cause and the severity of which can be investigated by means of further tests. An ECG and an echocardiogram are absolutely mandatory. According to the ESC guidelines (2016) the following laboratory tests are recommended for a patient with newly diagnosed HF in order to evaluate the patient’s suitability for particular therapies and to detect treatable causes and comorbidities: Hemoglobin and WBC - urea, creatinine (with estimated GFR), sodium, potassium, - glucose, HbA1c --lipid profile- liver function tests (AST, ALT, bilirubin,GGT) TSH - ferritin. Natriuretic peptides can also be cosidered as a part of the evaluation. Depending on the findings and the pretest probability of coronary artery disease (risk factors), coronary angiography is often indicated in cases of HF, especially with LV systolic dysfunction, to confirm or exclude coronary artery disease, as a common underlying cause.
On echocardiography this patient had a dilated and diffusely hypokinetic LV with an EF 35 % and also a dilated left atrium. The right heart chambers and the valves were without significant abnormalities (appart from moderate functional mitral regurgitation). Coronary angiography did not reveal significant coronary arterial stenoses. He was diagnosed with HFrEF due to dilated cardiomyopathy and treated with an ACE inhibitor (quinapril), a beta blocker (carvedilol), an MRA (eplerenone) and a loop diuretic (furosemide). Symptoms resolved and on re-evaluation after three months of treatment his EF had improved (40 %) and the dilatation of the LV had decreased. Subsequently, the dosage of the diuretic was reduced and the dosage of the ACE inhibitor was increased.
A reminder of relevant chest X ray anatomy :
In the posteroanterior chest radiograph the right border of the cardiomediastinal shadow is formed (from its lower to its upper parts), by the right atrium, the ascending aorta, and superior vena cava and further cranially it widens into a funnel shape, where its right border is formed by the brachiocephalic trunk. The upper margin of the left cardiomediastinal silhouette (from its upper to its lower portions) is formed by the aortic arch, the left pulmonary artery and the atrial appendage. The lower part of the left cardiomediastinal silhouette is formed by the left ventricle. The contour of the left hemidiaphragm is visible through the heart shadow almost as far as the shadow of the vertebral column.
Lateral chest x ray: The anterior cardiac border is formed by the right ventricle. and its upper part by the shadow of the aortic root continuing to the shadow of the aortic arch. The anterior surface of the right ventricle normally is in contact with the sternum along less than one-third of the length of the sternum
The cranial border of the middle mediastinum is defined by the shadow of the aortic arch. The shadow of the arch is interrupted by the radiolucent (black) band of the trachea and main bronchi. The lower part of the posterior heart border is formed by the left ventricle and its upper part by the left atrium.
A usual finding in patients with HF with reduced EF is an enlarged cardiac silhouette (cardiomegaly): In an inspiratory posteroanterior chest x ray the width if the cardiac silhouette is more than half of the width of the maximum internal diameter of the thorax. Cardiomegaly is almost always present in chronic systolic HF. In some forms of acute-new onset systolic HF, such as in the context of an acute myocardial infarction, cardiomegally often is not present (because the left ventricle did not have time to dilate), but there are signs of pulmonary congestion.
Clear signs of pulmonary congestion (elevated pulmonary venous pressure) are usually present in acute heart failure, but in much fewer patients with chronic heart failure. Such signs are
Upper lobe redistribution (enlarged upper lobe vessels in comparison to lower lobe vessels-in other words: prominence of upper lobe blood vessels. Normally, on the erect radiograph upper lobe vessels are less prominent and have a smaller diameter than lower lobe vessels.Important: The term redistribution applies to chest x-rays taken in full inspiration in the erect position),
Enlarged hilar shadows of the lungs (due to dilated pulmonary veins) and increased diameter of the pulmonary vessels,
Septal or Kerley B lines
[These lines-named after Peter Kerley, a radiologist from Ireland- are short, usually 1 -2 cm in length, parallel horizontal thin lines at the lung periphery, They represent thickened interlobular septa (because of interstitial edema, i.e increased interstitial fluid).They are parallel to one another, at right angles to the pleura. kerley B lines may be seen in any lung zone, but usually they are observed at the bases on the PA radiograph, and in the substernal region on lateral radiographs. The usual cause of Kerley B lines is interstitial pulmonary edema from congestive heart failure,. There are also other causes that can produce Kerley B lines by thickening of the septa between pulmonary lobules, such as pulmonary fibrosis, pneumoconiosis, lymphangitis carcinomatosa, malignant lymphoma, viral and mycoplasmal pneumonia.]
When fluid leaks into the peribronchovascular interstitium it is seen as thickening of the bronchial walls (peribronchial cuffing) and as loss of definition of hilar vessels (perihilar haze). Τhe above signs (Kerley B lines, peribronchial cuffing and perihilar haze) are signs of interstitial pulmonary edema (leakage of fluid into the interstitium of the lungs).and in more severe cases of congestion:
Alveolar pulmonary edema, due to leakage of fluid into the alveoli : Alveolar pulmonary edema is characterized by perihilar consolidations, i.e.large shadows or infiltrates (white areas like mist) surrounding the pulmonary hilae and air bronchograms within these consolidations. Air bronchogram is the appearance of air-containing bronchi within an area of consolidation, as branching radiolucent (=black) lines.
Pleural effusions are not rare in HF, often bilateral. In HF when there is a unilateral pleural effusion, it is usually on the right side.
Chest radiography in heart failure:
It is indicated for patients with suspected new-onset HF or with worsening HF. The goal is to assess heart size and to detect signs of pulmonary congestion, as well as to search for a possible pulmonary disease that may cause or contribute to the patient’s symptoms.A usual finding in patients with HF with reduced EF is an enlarged cardiac silhouette (cardiomegaly): In an inspiratory posteroanterior chest x ray the width if the cardiac silhouette is more than half of the width of the maximum internal diameter of the thorax. Cardiomegaly is almost always present in chronic systolic HF. In some forms of acute-new onset systolic HF, such as in the context of an acute myocardial infarction, cardiomegally often is not present (because the left ventricle did not have time to dilate), but there are signs of pulmonary congestion.
Clear signs of pulmonary congestion (elevated pulmonary venous pressure) are usually present in acute heart failure, but in much fewer patients with chronic heart failure. Such signs are
Upper lobe redistribution (enlarged upper lobe vessels in comparison to lower lobe vessels-in other words: prominence of upper lobe blood vessels. Normally, on the erect radiograph upper lobe vessels are less prominent and have a smaller diameter than lower lobe vessels.Important: The term redistribution applies to chest x-rays taken in full inspiration in the erect position),
Enlarged hilar shadows of the lungs (due to dilated pulmonary veins) and increased diameter of the pulmonary vessels,
Septal or Kerley B lines
[These lines-named after Peter Kerley, a radiologist from Ireland- are short, usually 1 -2 cm in length, parallel horizontal thin lines at the lung periphery, They represent thickened interlobular septa (because of interstitial edema, i.e increased interstitial fluid).They are parallel to one another, at right angles to the pleura. kerley B lines may be seen in any lung zone, but usually they are observed at the bases on the PA radiograph, and in the substernal region on lateral radiographs. The usual cause of Kerley B lines is interstitial pulmonary edema from congestive heart failure,. There are also other causes that can produce Kerley B lines by thickening of the septa between pulmonary lobules, such as pulmonary fibrosis, pneumoconiosis, lymphangitis carcinomatosa, malignant lymphoma, viral and mycoplasmal pneumonia.]
When fluid leaks into the peribronchovascular interstitium it is seen as thickening of the bronchial walls (peribronchial cuffing) and as loss of definition of hilar vessels (perihilar haze). Τhe above signs (Kerley B lines, peribronchial cuffing and perihilar haze) are signs of interstitial pulmonary edema (leakage of fluid into the interstitium of the lungs).and in more severe cases of congestion:
Alveolar pulmonary edema, due to leakage of fluid into the alveoli : Alveolar pulmonary edema is characterized by perihilar consolidations, i.e.large shadows or infiltrates (white areas like mist) surrounding the pulmonary hilae and air bronchograms within these consolidations. Air bronchogram is the appearance of air-containing bronchi within an area of consolidation, as branching radiolucent (=black) lines.
Pleural effusions are not rare in HF, often bilateral. In HF when there is a unilateral pleural effusion, it is usually on the right side.
Echocardiography: Useful indices of left ventricular systolic function
The most frequently used methods for the assessment of left ventricular (LV) systolic function are LV ejection fraction (EF) and regional wall motion analysis. Two dimensional (and also M-mode) echocardiography is the most common technique used but other tests that can examine LV systolic function are tissue Doppler imaging (TDI), speckle tracking imaging, three-dimensional (3D) echocardiography, computed tomography (CT), and cardiac magnetic resonance imaging (CMR).
M-mode echocardiography, which records the motion of cardiac structures in one dimension, can be used to obtain some indices of left ventricular (LV) systolic function. Measurements of LV dimensions are made in the parasternal long-axis view by positioning the cursor through the LV minor axis at the level of the tips of the mitral leaflets. Then fractional shortening (FS) can be calculated and even ejection fraction (EF) can be calculated with geometric assumptions (that are not accurate, if there are significant differences in regional contractile function, between various segments of the LV walls).
Stroke volume= the volume of blood ejected by a ventricle in systole= EDV-ESV.
The first step in the treatment of heart failure (HF) with reduced EF usually is starting three medications (an ACE-inhibitor, or an ARB, a beta blocker and a diuretic-see below). The diuretic is indicated if there are signs or symptoms of congestion, because it reduces symptoms, improves exercise tolerance and reduces the risk of hospitalization for HF. The ACE-inhibitor and the beta blocker are very important because they reduce mortality and the risk of HF hospitalization. ARBs are recommended only as an alternative (instead of an ACE inhibitor), in patients intolerant of an ACE-inhibitor.
Important: In every patient with ejection fraction (EF) ≤ 40 % there is a class I indication (i.e. a "strong and clear" indication) for treatment with an ACE-inhibitor, (or an ARB, if the first is not well tolerated) and a beta blocker, because this treatment reduces mortality (rates of death) and the rate of hospitalizations for HF.
Diuretics are clearly indicated in parients with HF (systolic or diastolic) if they have symptoms or signs of congestion and provide improvement of symptoms. They have not been shown in trials to reduce mortality.
Angiotensin converting enzyme (ACE) inhibitors are first line drugs in systolic heart failure (heart failure with reduced EF). ACE-inhibitors prevent conversion of angiotensin I to angiotensin II. This results in lower systemic vascular resistance (since angiotensin II induces vasoconstriction) and less secretion of aldosterone. Use of ACE inhibitors in patients with HFrEF increases survival, improves symptoms, decreases hospitalizations and improves left ventricular systolic function (the EF).
An Angiotensin receptor blocker (ARB) can be given instead, if the ACE inhibitor is not well tolerated by the patient. ARBs are specific antagonists to the angiotensin II type 1 receptors and so they act by inhibiting the effects of angiotensin II.
Absolute contraindications for an an ACE inhibitor or an ARB include pregnancy and bilateral renal artery stenosis. An absolute contraindication for an ACE inhibitor (and relative contraindication for an ARB) is a history of angioedema.
When using an ACE-inh or an ARB, caution is required in hyperkalemia (these drugs can cause elevation of potasium levels), in hepatic impairment, in renal dysfunction or unilateral stenosis of the renal artery (in this case there is a risk of causing deterioration of renal function), in aortic or mitral valve stenosis (risk of causing hypotension-if treament with these drugs is needed, one must be cautious to avoid rapid dose increments).
Relative contraindications for an ACE inhibitor or an ARB include hypotension (systolic blood pressure < 90 mm Hg), hyperkalemia (potassium > 5.5 mEq/L), severe renal insufficiency (creatinine > 3.0 mg/dL).
Unique side effects of ACE inhibitors are cough and angioedema. Chronic nonproductive cough associated with ACE inhibitors is caused by elevated levels of bradykinin. All attempts should be made to identify an alternative cause of cough before discontinuing the ACE inhibitor and replacing it with an ARB.
Angioedema is a rare complication of ACE inhibitors (0.4%) manifested by soft tissue edema of the lips, face, tongue, and, occasionally, the oro- pharynx and epiglottis. This rare complication typically begins in the first 2 weeks of ACE inhibitor therapy, but in some patients it presents months to years after starting therapy.
ARBs are used and monitored in the same manner as ACE inhibitors. ARBs have a similar side-effect profile to ACE inhibitors (e.g.they can induce hypotension, or occasionally they can induce renal insufficiency and hyperkalemia in some patients), but unlike ACE-inhibitors, ARBs do not induce cough and angioedema is a much more rare side effect with ARBs than with ACE inhibitors. Among ARBs, the best studied in patients with heart failure are valsartan and candesartan and they should be preferred.
Thus, in a symptomatic patient (NYHA II-IV) with HF with reduced left ventricular ejection fraction (EF<40%) according to the current guidelines (ESC-2016) initial treatment must include an ACE inh (or an ARB), a beta blocker and if there are symptoms or signs of congestion a diuretic (usually loop diuretic, e.g. furosemide).
The dose of the ACE inh (or ARB) and of the beta blocker should be gradually increased (up-titrated) to reach the evidence based dosage, or the maximum tolerated dosage below the evience based dosage. If the patient becomes asymptomatic no further medications are added (and we can consider reducing the diuretic dose).
If a patient with HF with reduced LVEF remains symptomatic (has symptoms NYHA II-IV) despite the above therapy with an ACE-inh and a beta blocker, then there is a clear indication to add a mineralocorticoid receptor antagonist (MRA). Thus, in this case treatment includes ACE-inh+beta blocker+MRA (+diuretic for symptoms or signs of congestion).
To summarize the indication of an MRA as mentioned in the guidelines : For patients who remain symptomatic (NYHA class II-IV) under treatment with diuretic+ACE inh. (or ARB) + beta blocker and also have an EF ≤ 35 %, a mineralocorticoid receptor antagonist (MRA) is added to this treatment scheme.
MRAs (spironolactone and eplerenone) are aldosterone antagonists, i.e. they prevent aldosterone from binding to its receptors. In such patients they reduce mortality and hospitalizations for HF.
Contraindications of aldosterone receptor antagonists (MRAs): potassium> 5 mmol / lt before the initiation of treatment, or severe renal failure: creatinine ≥2,5 mg / dL ,or calculated creatinine clearance ≤30 mL / min / 1,73 m2 body surface area.
For patients with EF ≤ 40% who remain symptomatic on treatment with a beta blocker, an ACE-inh. and a diuretic, if they cannot tolerate an MRA (or if this drug is contraindicated) an ARB can be added instead of the MRA and so treatment will include a beta blocker, an ACE-inh and an ARB (and a diuretic).
For patients with EF ≤ 40 % who cannot tolerate an ACE inh. because of cough, the treatment should include a beta blocker plus an ARB plus an MRA.
Note : A combination of three drugs blocking the renin-angiotensin-aldosterone axis, i.e. an ACE-inh plus an ARB plus an MRA should never be used, due to adverse effects.
For patients with systolic HF who remain symptomatic despite the above treatment (including a beta blocker, an ACE-inh or ARB, an MRA and a diuretic = 4 drugs) , if LVEF is ≤ 35 % and the patient can tolerate an ACE-inh or an ARB, then there is an indication to replace the ACE inh or ARB used in the above drug regimen with a new drug : ARNI (angiotensin receptor neprilysin inhibitor). Thus treatment includes then : beta blocker+ diuretic+ARNI+ MRA. ARNI is a new therapeutic class acting on the renin -angiotensin-aldosterone system (RAAS) and the neutral endopeptidase system. The first drug in this class is LCZ696, a molecule that combines the moieties of valsartan and sacubitril in a single substance. Sacubitril is a neprilysin inhibitor. By inhibiting neprilysin, the degradation of netriuretic peptides, bradykinin and other peptides is slowed and this has beneficial effects in the course of systolic HF, because natriuretic peptides enhance diuresis, natriuresis and myocardial relaxation, reduce the progress of adverse LV remodelling and inhibit renin and aldosterone secretion.
The addition of ivabradine to the above treatment is indicated to reduce hospitalization rates in patients with EF≤ 35 %, in sinus rhythm with heart rate ≥ 70 beats /minute who remain symptomatic, despite the above drug combination (including an evidence based ,or maximum tolerated dose of a beta-blocker combined with 2 inhibitory drugs of the renin-angiotensin-aldosterone axis: an ACE-inh or an ARB or ARNI plus an MRA / or an ACE inh plus an ARB). Ivabradine has an indication of class IIa.
2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure
Guidelines ESC Heart failure acute and chronic -2012
Fractional shortening (FS) is calculated from linear measurements
of LV dimensions from M-mode or 2D images:
FS = 100% × (LVDd – LVDs)/LVDd
where LVDd and LVDs are the LV end-diastolic dimension and
end-systolic dimension, respectively. FS normal values: 25-45 %
FS as an index of global LV function can be problematic when there is a marked difference in regional function, in patients with a previous myocardial infarction.
FS as an index of global LV function can be problematic when there is a marked difference in regional function, in patients with a previous myocardial infarction.
Two-dimensional (2D) echocardiography for the evaluation of LV systolic function
This is the primary mode for evaluation of LV systolic function. Endocardial border motion and wall thickening can be visualized and an experienced examiner can assess regional and global contractile function and roughly estimate the ejection fraction (EF) just by visualizing the LV in various echocardiographic views ("eyeball approach"). Quantitative measurements are obtained by tracing the endocardial border in end diastole and end systole in the apical 4- and 2-chamber views using the method of discs (modified Simpson rule). The machine software divides the LV along its long axis into a series of discs of equal height. Individual disc volume is calculated as height x disc area. LV volume is then calculated as the sum of disc volumes.
The ejection fraction (EF)= stroke volume/end diastolic volume.Stroke volume= the volume of blood ejected by a ventricle in systole= EDV-ESV.
(EDV= end diastolic volume, ESV= end systolic volume).
Thus, EF= (EDV-ESV)/ EDV.
Thus, EF= (EDV-ESV)/ EDV.
The left ventricular EF generally has a normal value ≥ 55%.
It is a measure of global LV systolic function, with established prognostic significance (the lower the EF, the worse the prognosis), but it is also influenced by preload, afterload, heart rate, and valvular function. (In patients with severe aortic or mitral regurgitation, conditions causing volume overload of the left ventricle, the normal value for the EF is ≥ 60%.) Systolic function of the left ventricle (LV) is considered as mildly reduced when EF is between 45 and 55 %, moderately reduced with EF between 30 and 45 % and severely reduced with EF< 30%.
Left ventricular EF is a strong predictor of clinical outcome and is widely used to make clinical decisions.
EF should be calculated from volumetric measurements
by 2D echocardiography. Even more accurate measurements of left ventricular volumes and EF are obtained with three dimensional (3D) echocardiography, or magnetic resonance imaging (MRI). The latter two techniques have similar accuracy.
SV= VTI (LVOT) x area (LVOT)
VTI is the velocity time integral (also named time velocity integral-TVI) of blood flow through the LVOT during systole.
This formula is explained as follows: VTI is calculated as the area under the curve of the Doppler velocity signal (which displays velocity on the vertical axis and time on the horizontal axis). This area of the Doppler signal is automatically calculated by the machine software, after the examiner manually traces the doppler velocity signal. It mathematically represents a velocity time integral, i.e. the sum of many products of velocity x time, each corresponding to every small time interval in systole. Since in every small time interval the column of blood moves by a distance given by the product of blood velocity x time interval, the VTI as a sum represents the total distance the column of blood has "traveled" in systole. This distance multiplied by the area of the orifice through which blood has passed, is the volume of blood which passed through the orifice in systole= the stroke volume (SV). Assuming a circular LVOT with radius r and diameter D (=2r) :
LVOT area = πr2=3,14r2=3,14(D/2)2 = (3,14 D2)/4= 0,785D2
In the absence of aortic regurgitation, SV reflects the forward effective blood flow in a cardiac beat and multiplied by heart rate (beats per minute) it gives the cardiac output (= the volume of blood passing through the circulation per minute). Strictly speaking, the SV is the hemodynamic result of LV function and not a true index of systolic function. Normal values of SV: 55-80 mL.
It is better to express the normal values of stroke volume per m2 of body surface area:
Normal values of SV(ml/m2): 26-54
The systolic annular velocity of the mitral valve (Sm) is a measure of left ventricular longitudinal contraction (contraction of the long axis oft the ventricle). It generally correlates well with the left ventricular EF. Normally Sm of the septal mitral annulus is > 6.5 cm/sec, and Sm of the lateral mitral annulus ≥ 8 cm/sec, when measured with pulse wave tissue doppler (PW-TDI). It is better to assess the mean Sm of the septal and lateral mitral annulus (normal value > 7.5 cm/sec). Note that myocardial velocities measured by the color TDI method are lower than velocities by pulsed Doppler (typically about 25% lower).
Early myocardial damage often involves the subendocardial fibres, with impairment in long-axis contraction occuring before changes in short-axis function. Thus, the Sm is a sensitive marker of mildly impaired left ventricular systolic function, even in people with apparently preserved systolic function and a normal EF, for example in those with diastolic heart failure, or in some diabetic patients without overt heart disease. Reduced annular TDI velocities are also present in subjects with hypertrophic cardiomyopathy, (even in people having the related gene mutations, who are at the stage of subclinical disease, with no cardiac hypertrophy).
Note that whereas the Sm velocity is an index of left ventricular systolic function, the Em or E΄velocity (the peak early diastolic mitral annular velocity, which is a negative wave) is an index of LV diastolic function and the Am or A΄velocity (an end-diastolic negative wave) is an index of the systolic function of the left atrium.
Kadappu KK, Thomas L. Tissue Doppler Imaging in Echocardiography: Value and Limitations.Heart, Lung and Circulation 2015;24:224-233
LINK Tissue Doppler Imaging in Echocardiography
Strain = L-Lo /Lo, where L is the current length and Lo is the original length of a myocardial segment.
Strain describes deformation (change in length) of the myocardium which occurs in three different directions, therefore there are three different types of strain, longitudinal (which is most often measured), circumferential and radial. Deformation in these three directions results from the different orientation of subepicardial and epicardial myofibers, that also generate a counterclockwise twist at the apex of the left ventricle and a clockwise twist at the base.
Strain rate (SR) is the rate of change of the strain value= the proportional change in length per unit of time. SR units are s-1
The normal value of the peak systolic strain (percentage of shortening) of the left ventricle during systole in the longitudinal axis is greater than 15%. To be more accurate, let us mention that normal peak systolic strain has a value more negative than -15%, usually between -15 and -25%. (The negative sign indicates a decrease in the length of the myocardium, i.e. shortening).
Peak systolic strain is influenced by preload (like the ejection fraction which is also influenced by the ventricular loading conditions) and can be used as an indicator of the total, and of the regional systolic function (when measured at a segment of the left ventricle).
The normal value for the peak systolic strain rate of the left ventricular myocardium is between - 1.2 and - 2 s-1 (sec-1=1/s).
In normal hearts the value of strain rate and strain is about the same in all myocardial segments from the base to the apex of the heart, (showing no significant difference). Conversely, myocardial velocity recorded by the tissue Doppler (in cm/s), and the displacement (change in position) of a given point of the myocardium (in mm) is greater in the basal portions and is getting smaller towards the apex.
An advantage of the percentage of myocardial deformation (strain) and of the rate of the proportional change in deformation (strain rate) is the following: Strain and strain rate is not affected by the translational motion of the heart ("bouncing" movements in the chest during systole). In contrast, the myocardial velocities recorded with tissue Doppler (TDI) are affected by the translational motion of the heart within the chest and not only by the motion of myocardial shortening in systole or lengthening in diastole.
A diminished peak systolic strain or strain rate is a sensitive marker of an impairment in systolic function.
Need more information about these modern echocardiographic techniques? In that case, here is a link for you to click on (free review article with the option to download PDF) ...
Strain and Strain Rate Imaging by Echocardiography – Basic Concepts and Clinical Applicability
Dandel Μ ,Lehmkuhl H, et al. Strain and Strain Rate Imaging by Echocardiography – Basic Concepts and Clinical Applicability. Current Cardiology Reviews, 2009, 5, 133-148.
It is a measure of global LV systolic function, with established prognostic significance (the lower the EF, the worse the prognosis), but it is also influenced by preload, afterload, heart rate, and valvular function. (In patients with severe aortic or mitral regurgitation, conditions causing volume overload of the left ventricle, the normal value for the EF is ≥ 60%.) Systolic function of the left ventricle (LV) is considered as mildly reduced when EF is between 45 and 55 %, moderately reduced with EF between 30 and 45 % and severely reduced with EF< 30%.
Left ventricular EF is a strong predictor of clinical outcome and is widely used to make clinical decisions.
EF should be calculated from volumetric measurements
by 2D echocardiography. Even more accurate measurements of left ventricular volumes and EF are obtained with three dimensional (3D) echocardiography, or magnetic resonance imaging (MRI). The latter two techniques have similar accuracy.
Doppler Echocardiography derived systolic indices (stroke volume)
Doppler echocardiography also provides some indices of LV systolic function, such as the stroke volume (SV), i.e. the blood volume ejected per beat. For this measurement one obtains from the apical 5 chamber view the pulse wave doppler signal of the velocity in the left ventricular outflow tract (LVOT) and also measures the diameter of the LVOT (in the parasternal long axis view at the base of the aortic valve leaflets or immediately proximal to the aortic valve).SV= VTI (LVOT) x area (LVOT)
VTI is the velocity time integral (also named time velocity integral-TVI) of blood flow through the LVOT during systole.
This formula is explained as follows: VTI is calculated as the area under the curve of the Doppler velocity signal (which displays velocity on the vertical axis and time on the horizontal axis). This area of the Doppler signal is automatically calculated by the machine software, after the examiner manually traces the doppler velocity signal. It mathematically represents a velocity time integral, i.e. the sum of many products of velocity x time, each corresponding to every small time interval in systole. Since in every small time interval the column of blood moves by a distance given by the product of blood velocity x time interval, the VTI as a sum represents the total distance the column of blood has "traveled" in systole. This distance multiplied by the area of the orifice through which blood has passed, is the volume of blood which passed through the orifice in systole= the stroke volume (SV). Assuming a circular LVOT with radius r and diameter D (=2r) :
LVOT area = πr2=3,14r2=3,14(D/2)2 = (3,14 D2)/4= 0,785D2
In the absence of aortic regurgitation, SV reflects the forward effective blood flow in a cardiac beat and multiplied by heart rate (beats per minute) it gives the cardiac output (= the volume of blood passing through the circulation per minute). Strictly speaking, the SV is the hemodynamic result of LV function and not a true index of systolic function. Normal values of SV: 55-80 mL.
It is better to express the normal values of stroke volume per m2 of body surface area:
Normal values of SV(ml/m2): 26-54
Tissue Doppler Imaging (TDI)
Measurement of mitral ring velocities or myocardial velocities of the basal segments (velocity of the movement of these tissues along the longitudinal axis of the heart) is a simple and sensitive method for the assessment of the left ventricular systolic and diastolic function. Both peak systolic (Sm) and early diastolic (Em) mitral annular or left ventricular basal velocities are nearly always reduced in patients presenting with the clinical syndrome of systolic heart failure.The systolic annular velocity of the mitral valve (Sm) is a measure of left ventricular longitudinal contraction (contraction of the long axis oft the ventricle). It generally correlates well with the left ventricular EF. Normally Sm of the septal mitral annulus is > 6.5 cm/sec, and Sm of the lateral mitral annulus ≥ 8 cm/sec, when measured with pulse wave tissue doppler (PW-TDI). It is better to assess the mean Sm of the septal and lateral mitral annulus (normal value > 7.5 cm/sec). Note that myocardial velocities measured by the color TDI method are lower than velocities by pulsed Doppler (typically about 25% lower).
Early myocardial damage often involves the subendocardial fibres, with impairment in long-axis contraction occuring before changes in short-axis function. Thus, the Sm is a sensitive marker of mildly impaired left ventricular systolic function, even in people with apparently preserved systolic function and a normal EF, for example in those with diastolic heart failure, or in some diabetic patients without overt heart disease. Reduced annular TDI velocities are also present in subjects with hypertrophic cardiomyopathy, (even in people having the related gene mutations, who are at the stage of subclinical disease, with no cardiac hypertrophy).
Note that whereas the Sm velocity is an index of left ventricular systolic function, the Em or E΄velocity (the peak early diastolic mitral annular velocity, which is a negative wave) is an index of LV diastolic function and the Am or A΄velocity (an end-diastolic negative wave) is an index of the systolic function of the left atrium.
Kadappu KK, Thomas L. Tissue Doppler Imaging in Echocardiography: Value and Limitations.Heart, Lung and Circulation 2015;24:224-233
LINK Tissue Doppler Imaging in Echocardiography
Myocardial strain and strain rate imaging
In general, in myocardial segments with diminished systolic function, systolic velocities are typically reduced and there are also reductions in systolic strain and strain rate. Strain is the proportion (percentage) of change in length of the myocardium (units %) and it is negative in systole, since there is a negative change in length (shortening), and positive in diastole (because in diastole the length increases).Strain = L-Lo /Lo, where L is the current length and Lo is the original length of a myocardial segment.
Strain describes deformation (change in length) of the myocardium which occurs in three different directions, therefore there are three different types of strain, longitudinal (which is most often measured), circumferential and radial. Deformation in these three directions results from the different orientation of subepicardial and epicardial myofibers, that also generate a counterclockwise twist at the apex of the left ventricle and a clockwise twist at the base.
Strain rate (SR) is the rate of change of the strain value= the proportional change in length per unit of time. SR units are s-1
The normal value of the peak systolic strain (percentage of shortening) of the left ventricle during systole in the longitudinal axis is greater than 15%. To be more accurate, let us mention that normal peak systolic strain has a value more negative than -15%, usually between -15 and -25%. (The negative sign indicates a decrease in the length of the myocardium, i.e. shortening).
Peak systolic strain is influenced by preload (like the ejection fraction which is also influenced by the ventricular loading conditions) and can be used as an indicator of the total, and of the regional systolic function (when measured at a segment of the left ventricle).
The normal value for the peak systolic strain rate of the left ventricular myocardium is between - 1.2 and - 2 s-1 (sec-1=1/s).
In normal hearts the value of strain rate and strain is about the same in all myocardial segments from the base to the apex of the heart, (showing no significant difference). Conversely, myocardial velocity recorded by the tissue Doppler (in cm/s), and the displacement (change in position) of a given point of the myocardium (in mm) is greater in the basal portions and is getting smaller towards the apex.
An advantage of the percentage of myocardial deformation (strain) and of the rate of the proportional change in deformation (strain rate) is the following: Strain and strain rate is not affected by the translational motion of the heart ("bouncing" movements in the chest during systole). In contrast, the myocardial velocities recorded with tissue Doppler (TDI) are affected by the translational motion of the heart within the chest and not only by the motion of myocardial shortening in systole or lengthening in diastole.
A diminished peak systolic strain or strain rate is a sensitive marker of an impairment in systolic function.
Need more information about these modern echocardiographic techniques? In that case, here is a link for you to click on (free review article with the option to download PDF) ...
Strain and Strain Rate Imaging by Echocardiography – Basic Concepts and Clinical Applicability
Dandel Μ ,Lehmkuhl H, et al. Strain and Strain Rate Imaging by Echocardiography – Basic Concepts and Clinical Applicability. Current Cardiology Reviews, 2009, 5, 133-148.
Treatment of systolic heart failure (HF with reduced ejection fraction)
The first step in the treatment of heart failure (HF) with reduced EF usually is starting three medications (an ACE-inhibitor, or an ARB, a beta blocker and a diuretic-see below). The diuretic is indicated if there are signs or symptoms of congestion, because it reduces symptoms, improves exercise tolerance and reduces the risk of hospitalization for HF. The ACE-inhibitor and the beta blocker are very important because they reduce mortality and the risk of HF hospitalization. ARBs are recommended only as an alternative (instead of an ACE inhibitor), in patients intolerant of an ACE-inhibitor.
Important: In every patient with ejection fraction (EF) ≤ 40 % there is a class I indication (i.e. a "strong and clear" indication) for treatment with an ACE-inhibitor, (or an ARB, if the first is not well tolerated) and a beta blocker, because this treatment reduces mortality (rates of death) and the rate of hospitalizations for HF.
Diuretics are clearly indicated in parients with HF (systolic or diastolic) if they have symptoms or signs of congestion and provide improvement of symptoms. They have not been shown in trials to reduce mortality.
Angiotensin converting enzyme (ACE) inhibitors are first line drugs in systolic heart failure (heart failure with reduced EF). ACE-inhibitors prevent conversion of angiotensin I to angiotensin II. This results in lower systemic vascular resistance (since angiotensin II induces vasoconstriction) and less secretion of aldosterone. Use of ACE inhibitors in patients with HFrEF increases survival, improves symptoms, decreases hospitalizations and improves left ventricular systolic function (the EF).
An Angiotensin receptor blocker (ARB) can be given instead, if the ACE inhibitor is not well tolerated by the patient. ARBs are specific antagonists to the angiotensin II type 1 receptors and so they act by inhibiting the effects of angiotensin II.
Absolute contraindications for an an ACE inhibitor or an ARB include pregnancy and bilateral renal artery stenosis. An absolute contraindication for an ACE inhibitor (and relative contraindication for an ARB) is a history of angioedema.
When using an ACE-inh or an ARB, caution is required in hyperkalemia (these drugs can cause elevation of potasium levels), in hepatic impairment, in renal dysfunction or unilateral stenosis of the renal artery (in this case there is a risk of causing deterioration of renal function), in aortic or mitral valve stenosis (risk of causing hypotension-if treament with these drugs is needed, one must be cautious to avoid rapid dose increments).
Relative contraindications for an ACE inhibitor or an ARB include hypotension (systolic blood pressure < 90 mm Hg), hyperkalemia (potassium > 5.5 mEq/L), severe renal insufficiency (creatinine > 3.0 mg/dL).
Unique side effects of ACE inhibitors are cough and angioedema. Chronic nonproductive cough associated with ACE inhibitors is caused by elevated levels of bradykinin. All attempts should be made to identify an alternative cause of cough before discontinuing the ACE inhibitor and replacing it with an ARB.
Angioedema is a rare complication of ACE inhibitors (0.4%) manifested by soft tissue edema of the lips, face, tongue, and, occasionally, the oro- pharynx and epiglottis. This rare complication typically begins in the first 2 weeks of ACE inhibitor therapy, but in some patients it presents months to years after starting therapy.
ARBs are used and monitored in the same manner as ACE inhibitors. ARBs have a similar side-effect profile to ACE inhibitors (e.g.they can induce hypotension, or occasionally they can induce renal insufficiency and hyperkalemia in some patients), but unlike ACE-inhibitors, ARBs do not induce cough and angioedema is a much more rare side effect with ARBs than with ACE inhibitors. Among ARBs, the best studied in patients with heart failure are valsartan and candesartan and they should be preferred.
A beta blocker (carvedilol, bisoprolol, or metoprolol sustained release tablets, or nebivolol) is initiated with a low dose.
The dosage of ACE inhibitor or ARB and beta-blocker (starting from a low dosage) should be gradually titrated to the evidence-based dose, used in the major trials, or to the maximum tolerated dose below the evidence based dose. Thus, in a symptomatic patient (NYHA II-IV) with HF with reduced left ventricular ejection fraction (EF<40%) according to the current guidelines (ESC-2016) initial treatment must include an ACE inh (or an ARB), a beta blocker and if there are symptoms or signs of congestion a diuretic (usually loop diuretic, e.g. furosemide).
The dose of the ACE inh (or ARB) and of the beta blocker should be gradually increased (up-titrated) to reach the evidence based dosage, or the maximum tolerated dosage below the evience based dosage. If the patient becomes asymptomatic no further medications are added (and we can consider reducing the diuretic dose).
If a patient with HF with reduced LVEF remains symptomatic (has symptoms NYHA II-IV) despite the above therapy with an ACE-inh and a beta blocker, then there is a clear indication to add a mineralocorticoid receptor antagonist (MRA). Thus, in this case treatment includes ACE-inh+beta blocker+MRA (+diuretic for symptoms or signs of congestion).
To summarize the indication of an MRA as mentioned in the guidelines : For patients who remain symptomatic (NYHA class II-IV) under treatment with diuretic+ACE inh. (or ARB) + beta blocker and also have an EF ≤ 35 %, a mineralocorticoid receptor antagonist (MRA) is added to this treatment scheme.
MRAs (spironolactone and eplerenone) are aldosterone antagonists, i.e. they prevent aldosterone from binding to its receptors. In such patients they reduce mortality and hospitalizations for HF.
Contraindications of aldosterone receptor antagonists (MRAs): potassium> 5 mmol / lt before the initiation of treatment, or severe renal failure: creatinine ≥2,5 mg / dL ,or calculated creatinine clearance ≤30 mL / min / 1,73 m2 body surface area.
For patients with EF ≤ 40% who remain symptomatic on treatment with a beta blocker, an ACE-inh. and a diuretic, if they cannot tolerate an MRA (or if this drug is contraindicated) an ARB can be added instead of the MRA and so treatment will include a beta blocker, an ACE-inh and an ARB (and a diuretic).
For patients with EF ≤ 40 % who cannot tolerate an ACE inh. because of cough, the treatment should include a beta blocker plus an ARB plus an MRA.
Note : A combination of three drugs blocking the renin-angiotensin-aldosterone axis, i.e. an ACE-inh plus an ARB plus an MRA should never be used, due to adverse effects.
For patients with systolic HF who remain symptomatic despite the above treatment (including a beta blocker, an ACE-inh or ARB, an MRA and a diuretic = 4 drugs) , if LVEF is ≤ 35 % and the patient can tolerate an ACE-inh or an ARB, then there is an indication to replace the ACE inh or ARB used in the above drug regimen with a new drug : ARNI (angiotensin receptor neprilysin inhibitor). Thus treatment includes then : beta blocker+ diuretic+ARNI+ MRA. ARNI is a new therapeutic class acting on the renin -angiotensin-aldosterone system (RAAS) and the neutral endopeptidase system. The first drug in this class is LCZ696, a molecule that combines the moieties of valsartan and sacubitril in a single substance. Sacubitril is a neprilysin inhibitor. By inhibiting neprilysin, the degradation of netriuretic peptides, bradykinin and other peptides is slowed and this has beneficial effects in the course of systolic HF, because natriuretic peptides enhance diuresis, natriuresis and myocardial relaxation, reduce the progress of adverse LV remodelling and inhibit renin and aldosterone secretion.
Contraindications and precautions regarding the use of ARNI (LCZ696)
Concomitant treatment with an ACE-inh , or an ARB is contraindicated. Coadministration with direct renin inhibitor (aliskiren) is also not recommended.
Contraindications include:
Hypersensitivity (allergy) to the active substance or ingredients
Second and third trimesters of pregnancy
History of angioedema related to a previous treatment with an ACE inhibitor or an ARB, or history of hereditary or idiopathic angioedema
Severe hepatic dysfunction or cholestasis
Treatment onset with ARNI should be at least 36 hours after discontinuation of treatment with ACE-inh (due to the potential risk of angioedema).
The addition of ivabradine to the above treatment is indicated to reduce hospitalization rates in patients with EF≤ 35 %, in sinus rhythm with heart rate ≥ 70 beats /minute who remain symptomatic, despite the above drug combination (including an evidence based ,or maximum tolerated dose of a beta-blocker combined with 2 inhibitory drugs of the renin-angiotensin-aldosterone axis: an ACE-inh or an ARB or ARNI plus an MRA / or an ACE inh plus an ARB). Ivabradine has an indication of class IIa.
Digoxin may be considered (indication of class IIb) to reduce the risk of HF hospitalization in patients with an EF ≤ 45% : 1) in sinus rhythm who are unable to tolerate a beta-blocker (ivabradine is an alternative in patients with symptomatic HF with reduced LVEF unable to tolerate a beta- blocker and sinus rate ≥70/min.), or 2) with persisting symptoms despite optimal treatment (with the above medications) or with atrial fibrilation and inadequately controlled ventricular response (ventricular rate).
It is not recommended for patients with a QRS duration < 130 ms.
The specific indications are as follows: CRT is recommended for symptomatic patients with HF in sinus rhythm with a QRS duration ≥ 130 ms and left bundle branch block (LBBB) and with LVEF ≤35% despite optimal medical treatment (a class I indication).
In patients with systolic HF, (HFrEF) with LVEF≤ 35% and symptoms despite optimal medical treatment : CRT should/may be considered (class II indication) if :
QRS ≥ 130 msec with non-LBBB in sinus rhythm, or
for patients in AF and QRS ≥ 130 msec with NYHA Class III–IV provided there is a strategy to ensure bi-ventricular capture, or the patient is expected to return to sinus rhythm.
CRT in patients with the above characteristics has been shown in trials to improve symptoms and reduce morbidity and mortality. Biventricular pacing (CRT) rather than right ventricular pacing is recommended for patients with systolic heart failure (HFrEF) regardless of NYHA class with an indication for ventricular pacing, because of high degree AV block in order to reduce morbidity. This also includes patients with AF.
to reduce the risk of sudden death and imrove survival are the following:
Primary prevention : In symptomatic patients (NYHA class II-III) with systolic HF an implantable cardioverter-defibrillator (ICD) is indicated if LVEF≤ 35%, despite ≥3 months of optimal medical treatment provided they are expected to survive longer than one year with good functional status. This indication is for sympomatic patients with EF≤ 35% who have:
a) ischemic heart disease but they did not have a myocardial infarction in the prior 40 days or
b) dilated cardiomyopathy DCM.
ICD implantation is not recommended in patients with HFrEF in NYHA class IV with severe symptoms refractory to pharmacological therapy because these patients will not have a survival benefit. Exceptions to this rule are patients with HFrEF class NYHA IV who are candidates for a treatment cabable of improving the course of their end stage HF, such as cardiac resynchronization treatment (CRT), a ventricular assist device, or cardiac transplantation.
For secondary prevention : If the patient has recovered after an episode of ventricular arrhythmia causing haemodynamic instability (ventricular tachycardia, or ventricular fibrillation) not due to an identifiable reversible cause and expected to survive for >1 year with good functional status.
An ICD in asymptomatic patients with systolic HF (HFrEF) is recommended in patients receiving optimal medical treatment with severe systolic dysfunction : LVEF ≤30% either of ischemic origin, who are at least 40 days after acute myocardial infarction, or of non-ischemic origin (with asymptomatic non-ischemic dilated cardiomyopathy).ICD is recommended in patients: a) with asymptomatic.
In patients with the above indications randomized controled trials have shown that an ICD prevents sudden death and prolonsg life.
As mentioned above, since the implantation of an ICD aims to increase survival, it is considered in the absence of other diseases likely to cause death within the following year.
Patients with systolic HF, with one of the above indications for ICD implantation, if they have οn the ECG a QRS duration ≥130 ms should be considered for a defibrillator with biventricular pacing, i.e. with cardiac resynchronization treatment (CRT-D= cardiac resynchronization treatment and defibrillator) rather than ICD.
Diuretics are recommended in patients with HFpEF or HFmrEF, who have symptoms or signs of congestion. They are effective in alleviating symptoms. A study has also shown improvement in NYHA class with candesartan.
Patients with HFpEF or HFmrEF should be screened for both cardiovascular and noncardiovascular comorbidities, which, if present, should be treated in order to improve symptoms, well-being and/or prognosis. For example these patients often have hypertension, diabetes mellitus, or coronary artery disease. These conditions, which are also known to cause diastolic dysfunction, should be diagnosed, their severity should be assessed and effectively treated. Coronary reperfusion should be considered if there is symptomatic coronary heart disease (angina), or in cases where significant ischemia is demonstrated by non invasive diagnostic tests, if ischemia is considered to be involved in symptom worsening.
An important note is that no treatment has yet been shown convincingly, to reduce mortality in patients with HFpEF or HFmrEF. Trials of ACE-inhs, ARBs, beta-blockers and MRAs have failed to show mortality reduction in patients with HFpEF or HFmrEF. However, there is an exception to that general rule : Nebivolol in older patients with HFrEF, HFpEF or HFmrEF, reduced the combined endpoint of death or cardiovascular hospitalization, with no significant association between treatment effect and left ventricular EF.
Patients with diastolic LV dysfunction often deteriorate in case of a tachycardia or tachyarrhythmia (because the duration of diastole is reduced). Then control of heart rate (eg with beta-blockers or diltiazem) or restoration of normal sinus rhythm (when possible) is an important aspect of treatment.
Cardiac resynchronization treatment (CRT),
i.e. the implantation of a biventricular pacemaker is generally recommended for patients with symptomatic systolic HF (despite optimal medical treatment), with a QRS duration is ≥ 130 ms (miliseconds) and left ventricular ejection fraction LVEF≤ 35%.It is not recommended for patients with a QRS duration < 130 ms.
The specific indications are as follows: CRT is recommended for symptomatic patients with HF in sinus rhythm with a QRS duration ≥ 130 ms and left bundle branch block (LBBB) and with LVEF ≤35% despite optimal medical treatment (a class I indication).
In patients with systolic HF, (HFrEF) with LVEF≤ 35% and symptoms despite optimal medical treatment : CRT should/may be considered (class II indication) if :
QRS ≥ 130 msec with non-LBBB in sinus rhythm, or
for patients in AF and QRS ≥ 130 msec with NYHA Class III–IV provided there is a strategy to ensure bi-ventricular capture, or the patient is expected to return to sinus rhythm.
CRT in patients with the above characteristics has been shown in trials to improve symptoms and reduce morbidity and mortality. Biventricular pacing (CRT) rather than right ventricular pacing is recommended for patients with systolic heart failure (HFrEF) regardless of NYHA class with an indication for ventricular pacing, because of high degree AV block in order to reduce morbidity. This also includes patients with AF.
Indications for an implantable cardioverter-defibrillator (ICD) in patients with heart failure
to reduce the risk of sudden death and imrove survival are the following:Primary prevention : In symptomatic patients (NYHA class II-III) with systolic HF an implantable cardioverter-defibrillator (ICD) is indicated if LVEF≤ 35%, despite ≥3 months of optimal medical treatment provided they are expected to survive longer than one year with good functional status. This indication is for sympomatic patients with EF≤ 35% who have:
a) ischemic heart disease but they did not have a myocardial infarction in the prior 40 days or
b) dilated cardiomyopathy DCM.
ICD implantation is not recommended in patients with HFrEF in NYHA class IV with severe symptoms refractory to pharmacological therapy because these patients will not have a survival benefit. Exceptions to this rule are patients with HFrEF class NYHA IV who are candidates for a treatment cabable of improving the course of their end stage HF, such as cardiac resynchronization treatment (CRT), a ventricular assist device, or cardiac transplantation.
For secondary prevention : If the patient has recovered after an episode of ventricular arrhythmia causing haemodynamic instability (ventricular tachycardia, or ventricular fibrillation) not due to an identifiable reversible cause and expected to survive for >1 year with good functional status.
An ICD in asymptomatic patients with systolic HF (HFrEF) is recommended in patients receiving optimal medical treatment with severe systolic dysfunction : LVEF ≤30% either of ischemic origin, who are at least 40 days after acute myocardial infarction, or of non-ischemic origin (with asymptomatic non-ischemic dilated cardiomyopathy).ICD is recommended in patients: a) with asymptomatic.
In patients with the above indications randomized controled trials have shown that an ICD prevents sudden death and prolonsg life.
As mentioned above, since the implantation of an ICD aims to increase survival, it is considered in the absence of other diseases likely to cause death within the following year.
Patients with systolic HF, with one of the above indications for ICD implantation, if they have οn the ECG a QRS duration ≥130 ms should be considered for a defibrillator with biventricular pacing, i.e. with cardiac resynchronization treatment (CRT-D= cardiac resynchronization treatment and defibrillator) rather than ICD.
Treatment of Heart Failure with preserved ejection fraction (HFpEF) and of Heart Failure with middle range ejection fraction (HFmrEF)
Diuretics are recommended in patients with HFpEF or HFmrEF, who have symptoms or signs of congestion. They are effective in alleviating symptoms. A study has also shown improvement in NYHA class with candesartan.
Patients with HFpEF or HFmrEF should be screened for both cardiovascular and noncardiovascular comorbidities, which, if present, should be treated in order to improve symptoms, well-being and/or prognosis. For example these patients often have hypertension, diabetes mellitus, or coronary artery disease. These conditions, which are also known to cause diastolic dysfunction, should be diagnosed, their severity should be assessed and effectively treated. Coronary reperfusion should be considered if there is symptomatic coronary heart disease (angina), or in cases where significant ischemia is demonstrated by non invasive diagnostic tests, if ischemia is considered to be involved in symptom worsening.
An important note is that no treatment has yet been shown convincingly, to reduce mortality in patients with HFpEF or HFmrEF. Trials of ACE-inhs, ARBs, beta-blockers and MRAs have failed to show mortality reduction in patients with HFpEF or HFmrEF. However, there is an exception to that general rule : Nebivolol in older patients with HFrEF, HFpEF or HFmrEF, reduced the combined endpoint of death or cardiovascular hospitalization, with no significant association between treatment effect and left ventricular EF.
Patients with diastolic LV dysfunction often deteriorate in case of a tachycardia or tachyarrhythmia (because the duration of diastole is reduced). Then control of heart rate (eg with beta-blockers or diltiazem) or restoration of normal sinus rhythm (when possible) is an important aspect of treatment.
Other treatment options for severe acute decompensated or chronic end stage heart failure with reduced EF.
Ventricular assist devices (VADs)
These devices are used for patients with acutely decompensated heart failure (HF) not responding to medical treatment and also for end-stage (ie, ACC/AHA stage D) chronic HF. Patients with end stage (stage D) heart failure have the following characteristics: severe symptoms at rest or with minimal activity despite optimal medical treatment, recurrent decompensation with hospitalizations, severe cardiac dysfunction and often a need for treatment with inotropes.
The left ventricle can be supported with a left ventricular assist device (LVAD), the right ventricle with a right ventricular assist device (RVAD), or both ventricles with a biventricular assist device (BiVAD). Another term for a VAD is a ventricular assist system (VAS).
The left ventricle can be supported with a left ventricular assist device (LVAD), the right ventricle with a right ventricular assist device (RVAD), or both ventricles with a biventricular assist device (BiVAD). Another term for a VAD is a ventricular assist system (VAS).
A LVAD can be placed temporarily in acute refractory left ventricular failure (for example in patients acute, severe myocarditis) as a bridge to recovery. This can be achieved by unloading the dysfunctional heart to allow reverse remodeling, i.e. reduction of the left ventricular (LV) dilatation and improvement in systolic function.
A VAD can also be used in patients with end-stage heart failure, either as a bridge to heart transplantation or for long term destination (permanent) treatment. A VAD as a destination therapy can be used in patients with end-stage heart failure, refractory to all other treatment options who are not transplant candidates and who otherwise would die without treatment..
For patients with end stage HF, destination therapy with LVADs compared to medical therapy has shown better results (than medical therapy) in terms of quality of life and longer survival. This has been shown in the REMATCH trial (Randomized Evaluation of Mechanical Assistance for the Treatment of Congestive Heart Failure) and also confirmed by newer data.
Potential complications of ventricular assist devices (VADs)
Potential complications of ventricular assist devices (VADs)
Although VADs improve survival and quality of life in patients with end-stage HF, complications can occur and patients need expert follow up. Potential complications include mechanical dysfunction, infection, bleeding, and thromboembolic events.
A Video: Echocardiography in advanced (end-stage ) heart failure with reduced EF. A concise introduction with a case presentation. The common echo findings. (To watch the video on a large screen, after you have started playing the video, click on the symbol [] at the lower right corner of the video.
For a detailed analysis of the management of HF, please use the links to heart failure-guidelines given at the bottom of this page.
Also see (LINK):
Heart failure and heart disorders caused by cancer teatment (cardio-oncology)
GO BACK TO THE HOME PAGE AND TABLE OF CONTENTS LINK :
CARDIOLOGY BOOK ONLINE-HOME PAGE AND TABLE OF CONTENTS
BIBLIOGRAPHY AND USEFUL LINKS ABOUT HEART FAILURE MANAGEMENT
Okwuosa IS, Princewill O, Nwabueze C, et al.The ABCs of managing systolic heart failure: Past, present, and future. Cleve Clin J Med. 2016 Oct;83:753-765.
Link : The ABCs of managing systolic heart failure: Past, present, and future.
Reed BN, Sueta CA .A practical guide for the treatment of symptomatic heart failure with reduced ejection fraction (HFrEF). Curr Cardiol Rev. 2015;11:23-32.
CARDIOLOGY BOOK ONLINE-HOME PAGE AND TABLE OF CONTENTS
BIBLIOGRAPHY AND USEFUL LINKS ABOUT HEART FAILURE MANAGEMENT
Okwuosa IS, Princewill O, Nwabueze C, et al.The ABCs of managing systolic heart failure: Past, present, and future. Cleve Clin J Med. 2016 Oct;83:753-765.
Link : The ABCs of managing systolic heart failure: Past, present, and future.
Reed BN, Sueta CA .A practical guide for the treatment of symptomatic heart failure with reduced ejection fraction (HFrEF). Curr Cardiol Rev. 2015;11:23-32.
LINK https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4347206/
Heart failure with preserved ejection fraction: pathophysiology, diagnosis, and treatment. European Heart Journal (2011) 32, 670–679.
LINK https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3056204/pdf/ehq426.pdf
Sanderson J E. Heart failure with a normal ejection fraction.Heart 2007;93:155-158. doi:10.1136/hrt.2005.074187
Rose-Jones LJ, Rommel JJ, Chang PP. Heart failure with preserved ejection fraction: an ongoing enigma. Cardiol Clin. 2014; 32:151-61.
Heart failure with preserved ejection fraction: pathophysiology, diagnosis, and treatment. European Heart Journal (2011) 32, 670–679.
LINK https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3056204/pdf/ehq426.pdf
Sanderson J E. Heart failure with a normal ejection fraction.Heart 2007;93:155-158. doi:10.1136/hrt.2005.074187
Rose-Jones LJ, Rommel JJ, Chang PP. Heart failure with preserved ejection fraction: an ongoing enigma. Cardiol Clin. 2014; 32:151-61.
2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure
Guidelines ESC Heart failure acute and chronic -2012
ACC/AHA Guidelines Heart failure -2013
Classification of the cardiomyopathies: a position statement from the european society of cardiology
2014 ESC Guidelines on diagnosis and management of hypertrophic cardiomyopathy
2014 ACC/AHA Guideline on Perioperative Cardiovascular Evaluation and Management of Patients Undergoing Noncardiac Surgery
2014 ESC/ESA Guidelines on non-cardiac surgery: cardiovascular assessment and management
ESC Guidelines for the management of grown-up congenital heart disease
ACC/AHA 2008 Guidelines for the Management of Adults With Congenital Heart Disease
2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension
2014 ESC Guidelines on the diagnosis and management of acute pulmonary embolism
Classification of the cardiomyopathies: a position statement from the european society of cardiology
2014 ESC Guidelines on diagnosis and management of hypertrophic cardiomyopathy
2014 ACC/AHA Guideline on Perioperative Cardiovascular Evaluation and Management of Patients Undergoing Noncardiac Surgery
2014 ESC/ESA Guidelines on non-cardiac surgery: cardiovascular assessment and management
ESC Guidelines for the management of grown-up congenital heart disease
ACC/AHA 2008 Guidelines for the Management of Adults With Congenital Heart Disease
2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension
2014 ESC Guidelines on the diagnosis and management of acute pulmonary embolism
Advertisement